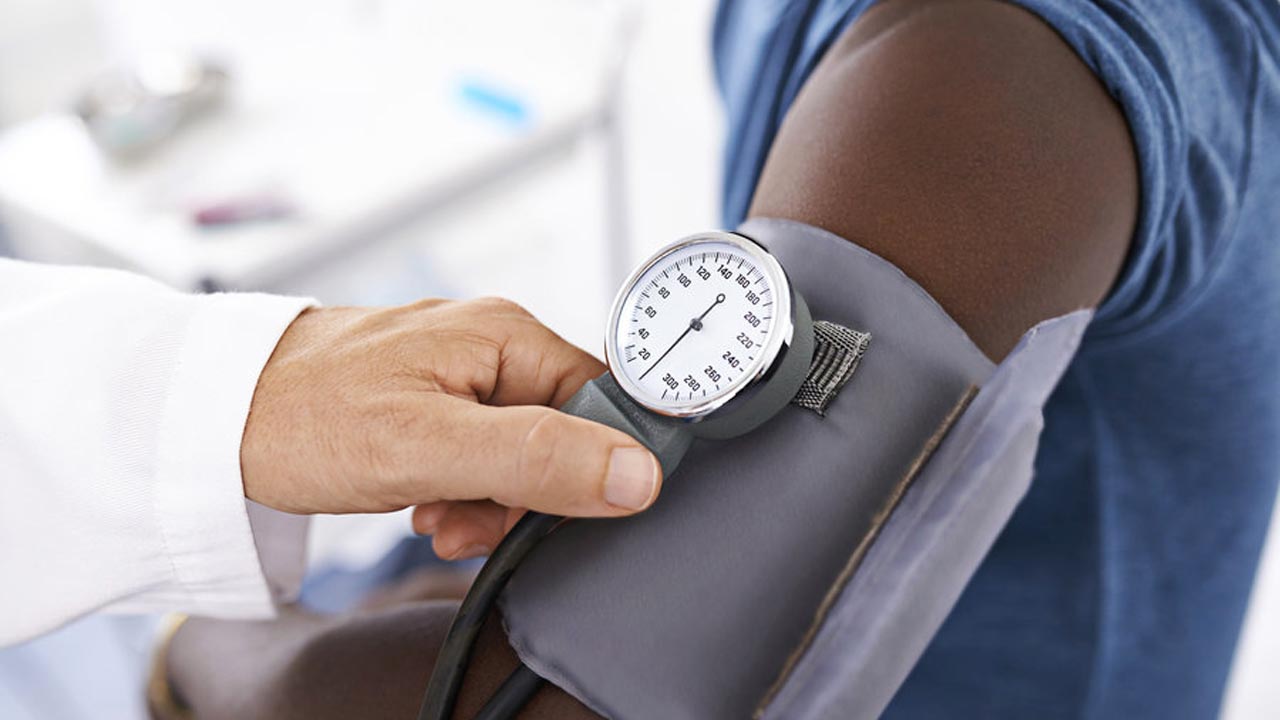
A new study has indicated that heart conditions such as coronary artery disease and cardiovascular risk factors such as diabetes and high cholesterol have a stronger connection with the decline in memory and thinking skills for middle-aged women than men.
The study published by Neurology – a medical journal of the American Academy of Neurology, also noted that the risk factors are higher for women despite a higher prevalence of those conditions in men.
Reacting to the study, Consultant Cardiologist at the Lagos State University Teaching Hospital, Ikeja, Dr. Ramon Moronkola said its findings have further validated previous related research on cardiovascular risk factors in middle age.
The study involved 1,857 individuals who were between the ages of 50 and 60, without dementia, at the beginning of the study.
The individuals were given a clinical evaluation every 15 months for an average of 3 years. The evaluation included 9 tests in executive function, language, memory, and spatial skills combined to calculate a composite cognitive score.
About 1,465 of the individuals had at least one cardiovascular condition or risk factor, with about 83 per cent of men compared with about 75 per cent of women.
The study author, Dr. Michelle Mielke of Mayo Clinic in Rochester, Minnesota, said the results show that midlife cardiovascular conditions and risk factors were associated with midlife cognitive decline.
Mielke, who is also a member of the American Academy of Neurology said:
“Specifically, we found that certain cardiovascular conditions, such as diabetes, heart disease and dyslipidemia, which is abnormally high levels of fats in the blood, had stronger associations with cognitive decline in women compared to men.”
The researchers found that most cardiovascular conditions were more strongly associated with cognitive functions among women. Heart disease was associated with more than a two-fold greater decline in composite cognitive test scores for women compared with men.
They also found that abnormally high levels of fat in the body, diabetes and heart disease were associated with language score declines only in women.
However, investigators also found that congestive heart failure was associated with language score declines only in men.
According to Mayo Clinic, the most common heart attack symptom in women is the same as in men — some type of chest pain, pressure or discomfort that lasts more than a few minutes or comes and goes.
The online health portal equally noted that chest pain is not always severe or even the most noticeable symptom, particularly in women.
“Women often describe heart attack pain as pressure or tightness. And it’s possible to have a heart attack without chest pain.
“Women are more likely than men to have heart attack symptoms unrelated to chest pain, such as neck, jaw, shoulder, upper back or upper belly (abdomen) discomfort, shortness of breath,” it said.
Other symptoms are a pain in one or both arms, nausea or vomiting, sweating, lightheadedness or dizziness, unusual fatigue and heartburn (indigestion).
It added that these symptoms may be vague and not as noticeable as the crushing chest pain often associated with heart attacks.
“This might be because women tend to have blockages not only in their main arteries but also in the smaller ones that supply blood to the heart — a condition called small vessel heart disease or coronary microvascular disease.
“Compared with men, women tend to have symptoms more often when resting, or even when asleep Emotional stress can play a role in triggering heart attack symptoms in women.
“Because women’s heart attack symptoms can differ from men’s, women might be diagnosed less often with heart disease than are men. Women are more likely than men to have a heart attack with no severe blockage in an artery (nonobstructive coronary artery disease.)”
Commenting further on the study, Dr. Moronkola stressed that some of the findings in the study have been demonstrated by earlier studies but noted that most of them did not assess the sex difference in the effect of the cardiovascular risk factor on cognitive decline.
The cardiologist explained that cognitive decline refers to impairment in some brain-based skills which are needed for the acquisition of knowledge, manipulation of information and reasoning.
“These skills naturally decline with age but the rate of decline is worse in individuals with cardiovascular risk factors. This means people with hypertension, diabetes, abnormal lipid level, etc will suffer faster decline than others.
“Even though more men suffer cardiovascular disease than females, this study found that these cardiovascular factors affected the females more than males.
“This finding must have been surprising to the researchers as one would have thought that the protective factors of the female hormones on the cardiovascular disease would have extended to preventing cognitive decline in females.
“Level of education has been shown to also affect the rate of decline in cognitive function with age and some epidemiological studies have shown that women tend to have a lower level of education than their male counterparts. This may be one of the reasons for the above findings,” Moronkola said.
He, however, said more studies will be needed to corroborate or refute the findings from the study.